Mastitis Spectrum- Blocked Ducts, Milk Blebs and Abscesses
Article Update: June 2025
MY BREAST IS SORE. WHAT SHOULD I DO?
A part of your breast feels lumpy, tender or painful. You may also have noticed a colour change (looking more red or purple) on that area of the breast. You may be wondering if you have a blocked duct or mastitis.
Whatever the reason for your sore breast:
1. Breastfeed as often as your baby wishes.
2. Rest.
3. Apply cold packs to the lumpy or tender area.
4. In consultation with your healthcare provider, consider using Ibuprofen alternating with Paracetamol.
Breastfeeding experts used to think of mastitis, blocked ducts, abscesses and milk blisters/“blebs” as separate problems in the breasts. Newer research suggests these are all stages of inflammation – the body’s response to a threat. The Academy of Breastfeeding Medicine (ABM) has revised their protocol explaining this: ABM Protocol #36, pdf The Mastitis Spectrum. This article is based on Protocol # 36 and some tried and proven La Leche League information.

MASTITIS
You may notice a large area of your breast that feels lumpy, swollen, hot and painful. The skin over that area may look red or darker than usual. You may get a high temperature or feel unwell like you have the ‘flu’, sometimes having a headache and tender muscles. These are all symptoms of inflammation in the breasts, commonly referred to as mastitis. Mastitis can make you feel very sick. It helps to start the suggestions in the box as soon as possible.
BLOCKED DUCTS
Blocked ducts refers to earlier symptoms of breast inflammation, or mastitis spectrum. The ducts or tubes (which carry milk from the glands in the breast to the nipple) or the tissue around them can become inflamed. If this happens, you may notice a lumpy or swollen area on your breast, or it may feel tender or sore.
MILK BLEBS OR BLISTERS
A milk blister, or bleb, refers to a painful white dot on the nipple or areola. This can be the result of inflammation or early mastitis in the breast which sends inflammatory cells from the milk tubes (ducts) to the surface of the nipple.
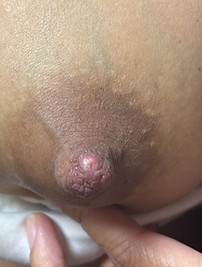



Milk blebs, blocked ducts and mastitis are all different stages of breast inflammation. Similar treatment helps all these conditions.
WHAT CAN I DO?
1. CONTINUE TO BREASTFEED YOUR BABY
None of these conditions are contagious to the baby. In fact certain milk components, like secretory IgA, a very important antibody, increases during periods of breast inflammation.
Breastfeed as often as your baby wishes. It is important for your baby to continue breastfeeding from the affected side to help prevent the inflammation from worsening and creating an abscess.
Ensure a deep comfortable latch. Call a La Leche League Leader if you need help with positioning and latching more comfortably. It may help to start the feed from the less sore side. Switch to the sore side after your milk has let down. This should then be less painful. Starting each feed on the same side for a few days should not be a problem.
If you are separated from your baby or if your baby refuses to breastfeed from the sore side, cold packs will help ease the discomfort from the excessive fullness. If you need to, express or pump just a little milk till you feel comfortable.
2. REST
Consider yourself sick, and rest! We can’t pour from an empty cup. Focus on caring for yourself, your breast, and your baby. Resting is important to help your body to heal.
Ask family members and friends for help with preparing food for the family, caring for other children or taking care of essential chores. Allow yourself the grace to rest.
Try to lie down while breastfeeding.
Keep supplies such as nappies and wipes, toys, books, your phone, water, and some snacks near you to minimise trips out of bed.
3. USE COLD (NOT ICE) PACKS ON THE SORE AREA
Apply cold packs to the sore area of the breast. Do not apply the cold pack onto the nipple or areola if you have a milk blister, rather to the closest part of the breast near the areola.
Applying cold packs frequently (as often as hourly for 5-10 minutes during the day) can be very helpful to settle the inflammation in the breast. During the night, having a cooler bag at hand next to the bed with the cold packs, will prevent you from having to get out of bed. During the night, the cold packs can be applied for 5 mins after each night time breastfeed.
If you don’t have cold packs, you could try a bag of frozen vegetables, or a cold face cloth or cold towel.
4. USE ANTI-INFLAMMATORY PAIN MEDICATION
The Academy of Breastfeeding Medicine Protocol on Mastitis recommends the use of high dose Ibuprofen (400-800mg) every 6 to 8 hours for a few days as an anti-inflammatory. This can be used in conjunction with Paracetamol to help with pain. Discuss any medication use with your healthcare provider. This article does not replace medical advice by your doctor.
5. SKIN-TO-SKIN CARE
Skin-to-skin care helps both your and your baby’s microbiome and provides protection against infection.
Most mastitis and blocked ducts will resolve or significantly improve after 48 hours of following these measures. If you feel better, you may need to continue these measures for a few more days till symptoms resolve. If however, things feel worse after 24-48 hours please consult your doctor.
DON'T I NEED ANTIBIOTICS?
Be aware that antibiotics may not be recommended right away. This is not an infection when it starts. Taking unnecessary antibiotics too early may encourage resistant strains of bacteria to thrive and may make you more likely to have recurrent mastitis or an abscess in the future. However, if you have tried steps 1-5 above for 48 hours and feel worse, you need to consult your doctor and antibiotics may then be prescribed if the breast inflammation has progressed to an infection. Even when an infection is present, it is safe to continue breastfeeding your baby. Your breastmilk has immune factors that protect the baby. Antibiotics for mastitis or breast abscesses are compatible with breastfeeding.
WHAT ABOUT ULTRASOUND FOR BLOCKED DUCTS AND MASTITITS?
Many areas do not have this technology available, and the evidence for therapeutic ultrasound (TUS) is not very strong. If TUS is available in your area, it may be helpful to relieve some oedema (swelling and extra fluid in the breast) and reduce inflammation. However, TUS provided by inexperienced practitioners may also increase inflammation in the breast and exacerbate the situation.
WHAT ABOUT LECITHIN SUPPLEMENTS?
Lecithin acts as an emulsifier, mixing the fattier and watery components of expressed breastmilk. However, the evidence for this supplement being used for breast inflammation is not strong.
WHAT ABOUT STEROID OINTMENTS?
The use of moderate potency topical steroids (e.g. Mometasone ointment) on nipple blebs can be helpful and may be a useful additional treatment according to the new ABM Mastitis protocol.
WHY DID I DEVELOP BREAST INFLAMMATION (BLOCKED DUCT/BLEB/MASTITIS)?
Possible contributing factors for breast inflammation include:
-
Latching and positioning which is not deep enough and comfortable.
-
Missing feeds, infrequent feeds, scheduling feeds or restricting the length of feeds
(This can also occur when weaning takes place too rapidly).
-
When a mother is making more breastmilk than her baby needs (for example by pumping or using galactagogues).
-
Excessive pumping and the use of silicone milk catching devices cause hyperlactation and breast inflammation. Chronic engorgement, over pumping (e.g. to build a freezer stash of expressed milk) or trying to “empty the breasts” can cause dysbiosis (an imbalance of microbes in the breasts) and all these factors increase the risk of mastitis.
-
Exclusively pumping can also affect the breast microbiome, since there is no feedback from saliva in the baby’s mouth to the nipple. Pump suction pressures may be higher or lower than the infant’s suction when feeding at the breast. Suction pressures that are too high can lead to breast and nipple trauma and inflammation, increasing the risk of mastitis. Suction pressures that are too low can lead to breast inflammation due to insufficient milk removal. Pumps do not remove milk as efficiently as a deeply latched baby feeding directly from the breast and may contribute to breast dysbiosis.
-
The use of nipple shields prevents deep latching and changes the microbiome of the breast. Nipple shields, pacifiers and other artificial nipples can also affect how babies suck.
-
The use of bottles and pacifiers also affect the microbiome and stimulate low grade inflammatory processes. If you are trying to minimise pump, nipple shield, and pacifier usage, it can be useful to discuss this with an LLL Leader.
-
Milk blisters can also result from friction from poorly fitted breast pump flanges. Avoid opening a milk blister yourself. It may bring some relief, but it also brings a risk of infection, more inflammation, and the possibility it will re-form. Avoid using soap or other cleansers on the nipple, as this can cause skin damage and pain.
-
Pressure on the milk ducts: This could include a bra (or an underwire) that’s too tight, restrictive clothing, car seat belts, backpack or baby carrier straps.
-
Certain injuries can result in sore breasts, such as being kicked or hit by an active toddler, or biting the breast.
-
Prior breast surgery, breast lumps, or injury to the breast can also hamper milk flow and increase the risk of inflammation.
-
There is some evidence that mastitis is more common in women who have recently taken antibiotics. Mothers who test positive for group B strep and those who have caesarean births may be given antibiotics during their labour and birth. This causes changes in the breast microbiome and may lead to an imbalance or “dysbiosis” which sets off breast inflammation. Direct breastfeeding rather than pumping, and skin to skin care can help your and the baby’s microbiome.
CERTAIN TREATMENTS MAY WORSEN BREAST INFLAMMATION AND SHOULD BE AVOIDED:
-
Applying heat to the breast, or soaking in warm water
-
Vigorous, deep massage, or squeezing to try to get rid of a blocked duct
-
Using a comb, vibrator, or electric toothbrush on the breast
-
Trying to “empty” the breast through extra pumping
-
Using antibiotics right at the beginning of symptoms
-
Using Epsom salts in a Haakaa or similar silicone breast pump for nipple blebs
-
Removing the skin or “popping” a bleb, which may allow infection to develop
A FEW WORDS ABOUT BREAST ABSCESSES
A breast abscess is a build-up of pus that is walled off in the breast. This can happen when a breast infection is not treated well. A small percentage of mastitis cases may progress to develop an abscess. A well-defined area may feel swollen, hard and painful (although very deep abscesses may not be painful). If you have mastitis that is not getting better, it is vital to see your doctor. If you have a breast abscess, your doctor is likely to recommend antibiotics and rest.
In some cases, the abscess will open up spontaneously and drain itself through the skin.
However, you may need to have the abscess drained surgically if symptoms don’t improve. A physician (usually a radiologist or a breast surgeon) will draw out the contents of the abscess with a needle aspiration, which may have to be repeated several times.

Milk and fluid leaking from a breast abscess after surgical incision
In certain cases, surgery under anaesthesia is necessary. A drain is usually inserted after a surgical cut has been made. The drain will stay in place until the abscess fluids have drained completely. Milk often drains from this wound until the wound heals up.
This does not mean the end of breastfeeding. No matter how your abscess is taken care of, continued breastfeeding on the affected breast is valuable in decreasing inflammation. If the abscess is so close to the nipple that your baby can’t latch on that side, you will need to express your milk. A temporary drop in milk production on the interrupted side will happen, but your other breast will increase milk production according to how frequently your baby drinks on that breast. Once the wound is healed, you can resume breastfeeding on the affected side again, and milk production will increase on that side again.
It can be useful to discuss the options for your individual situation with a La Leche League Leader.
A video on blocked ducts and mastitis:
EXTRA READING AND ADDITIONAL RESOURCES
If you would like to read more about the causes of mastitis, here is a good review: Interventions for the prevention of mastitis following childbirth | Cochrane
Since much of the information in the most recent ABM mastitis protocol is new, you may find it helpful to share it with your healthcare provider: ABM Protocol #36: https://www.bfmed.org/assets/ABM%20Protocol%20%2336.pdf
https://www.lllc.ca/mastitis-matter-inflammation
https://llli.org/breastfeeding-info/mastitis/
https://www.breastfeeding.asn.au/resources/mastitis
https://www.breastfeeding.asn.au/resources/breast-inflammation
https://breastfeeding.support/blisters-on-nipples/
https://physicianguidetobreastfeeding.org/mythbusters/blebs-mythbusters/
Maintaining Breastfeeding During the Treatment of Breast Abscesses Is Not Contraindicated
Tianzhu Long, Ziyu Ning, Benjie Fu, Yuzhi Yao, Ling Wu, Jiayue Luo, Zeyu Lin, and Hongmin Ma
Breastfeeding Medicine 2022 17:9, 753-757

